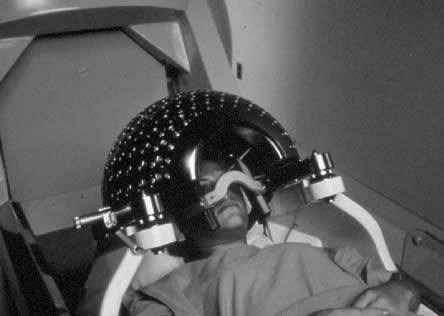
Gamma Knife
Gamma Knife® is a radiation therapy device. It uses advanced imaging and computer software to treat small targets in the head and brain. The device delivers an intense radiation dose to the target area while sparing surrounding brain tissue.
A radiation oncologist, medical physicist, and neurosurgeon will team up to identify the targets and provide your treatment. The medical physicist will ensure your safety by testing the machine and verifying that the computers and software are correct and acceptable.
What is the Gamma Knife used for?
Gamma Knife® helps find and precisely treat small targets in the head and brain. The device can deliver an intense dose of radiation to the target area while sparing surrounding brain tissue. Your doctor may use it to treat:
- malignant tumors that start in or spread to the brain
- benign brain tumors
- blood vessel defects and functional problems.
See the Brain Tumor, Brain Tumor Treatment, and Vascular Malformations pages for more information.
Doctors are studying possible uses of Gamma Knife® for epilepsy and Parkinson’s disease.
How does the Gamma Knife work?
Gamma Knife® uses Stereotactic Radiosurgery. This technique uses multiple beams of radiation converging in three dimensions to focus precisely on a target area. This allows your doctor to safely deliver an intense dose of radiation to that target. Many devices can move the patient in tiny increments during treatment to successfully focus radiation on all parts of the target.
Treatments using the Perfexion Device
Most Perfexion treatments take just one session. Targets larger than three or four centimeters often require more than one session.
Under local anesthesia, the doctor attaches a special rigid head frame to the patient's skull with four screws. The frame uses a three-dimensional coordinate system to help treatment planning. The doctor will use magnetic resonance imaging (MRI), computed tomography (CT), or angiography to obtain the necessary images. The images then go to the planning computer system. The treatment team will outline the target areas and normal anatomical structures. The computer will determine the exact spatial relationship between the target, normal structures, and the head frame. The team uses this information to calculate treatment parameters. Often, it is best to treat targets with combinations of several successive highly focused treatments (shots). The team fine-tunes the treatment parameters until they arrive at an optimal and conformal plan.
Using the planning coordinates, the doctor attaches the frame to the Gamma Knife® unit. The team centers the target in about 200 precision-aimed, converging gamma radiation beams. Treatment takes from several minutes to a few hours depending on the target’s shape and size, number of shots, and prescribed dose. Patients do not feel the radiation during treatment, but they may see flashes of light. After treatment, the doctor removes the frame, and the patient returns to normal activity.
Treatments using the Icon Device
Icon treatments differ from Perfexion treatments in that:
- Treatments take place in single or multiple sessions.
- The patient does not need an external frame.
- Icon uses a combination of onboard stereotactic Cone Beam CT imaging and real-time infrared motion detection and management. This allows Icon to achieve 0.15 mm treatment accuracy without a rigid frame.
See the Stereotactic Radiosurgery page for additional information.
Who operates the equipment?
A team approach provides patients with the greatest safety. This team usually consists of a radiation oncologist, medical physicist, and neurosurgeon specially trained to use a Gamma Knife®. Sometimes, a radiologist or neuroradiologist may also contribute input. Nursing staff, anesthesiologists (for patients who are unable to cooperate, such as children), and radiation therapists support the team. Together, these professionals work to provide high-quality care.
The Nuclear Regulatory Commission requires an “authorized user” (usually a radiation oncologist) to be at the treatment console during the entire procedure.
How is safety ensured?
Accurate placement of the shots is critical to localizing the radiation within a fraction of a millimeter. Anything less is unacceptable. In fact, the following are all critical to accurate treatment:
- Rigidly and accurately attaching the head frame
- Accurate targeting of imaging exams
- Shaping the volume of the target area (shot size, number, and relative intensity)
Correct target selection and accurate calculation of the amount of radiation to deliver are essential to successful treatment. A qualified medical physicist assures that the imaging and treatment planning computers and software are correct and acceptable. The physicist routinely tests the machine to ensure the safety of patients and medical staff.
This page was reviewed on August 30, 2023